Posts Tagged ‘psychosis’
Study: Automated VR psychotherapy can help reduce anxiety and distress, especially among those with psychosis and severe agoraphobia
Oxford University VR spinout demonstrates significant psychotherapy benefits in Lancet study (Fierce Healthcare): Virtual reality can help treat symptoms in patients with psychosis, according to a new study published in The Lancet Psychiatry. GameChangeVR automates psychotherapy, guiding users with a virtual coach. It was developed by OxfordVR, a digital therapeutics company, the University of Oxford…
Read MoreDoes marijuana use cause schizophrenia? (unclear, but unlikely)
Does Marijuana Use Cause Schizophrenia? (The New York Times): “… The concern is focused largely on the link between heavy usage and psychosis in young people. Doctors first suspected a link some 70 years ago, and the evidence has only accumulated since then. In a forthcoming book, “Tell Your Children,” Alex Berenson, a former Times reporter,…
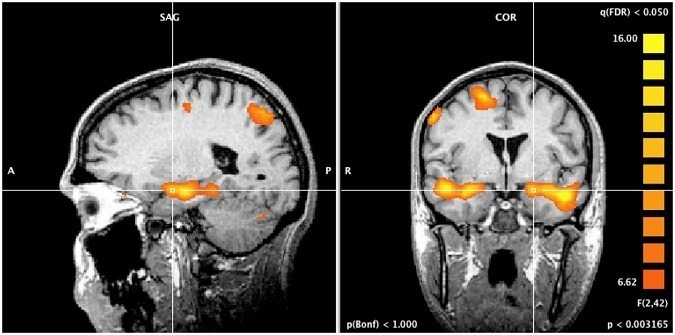
Read MoreStudy: Cognitive Behavioral Therapy (CBT), not medication, drives long-term rewiring of the brain to help reduce psychosis symptoms
Talking therapy changes the brain’s wiring, study reveals for first time (ScienceDaily): “A new study from King’s College London and South London and Maudsley NHS Foundation Trust has shown for the first time that cognitive behaviour therapy (CBT) strengthens specific connections in the brains of people with psychosis, and that these stronger connections are associated…
Read MoreCognitive Enhancement via Pharmacology AND Neuropsychology, in The New Executive Brain
(Editor’s Note: given the growing media attention to three apparently separate worlds ‑cognitive enhancement via drugs, brain fitness training software, computerized neurocognitive assessments‑, I found it refreshing to see our co-founder Elkhonon Goldberg introduce the topic of cognotropic drugs with an integrative perspective in the much updated new edition of his classic book, now titled…
Read More