Alphabet’s X shares Amber EEG system to expand the quest for mental health biomarkers
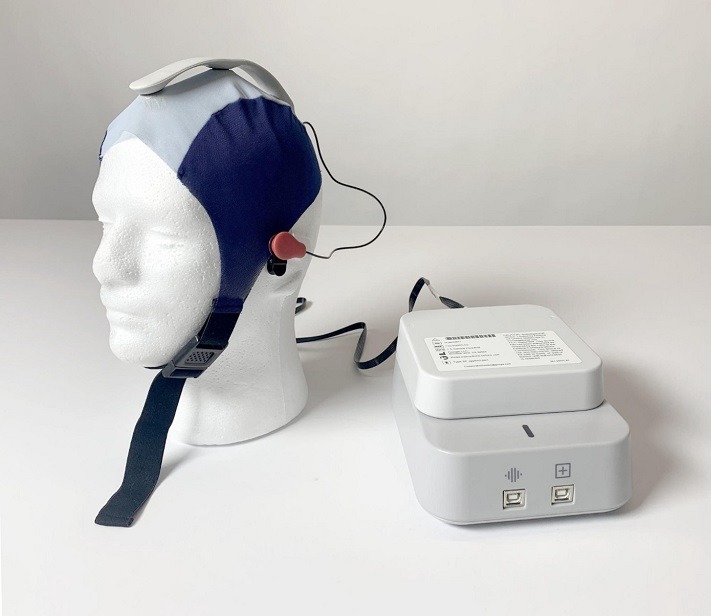
Amber’s final EEG prototype: Headset, sensor strip and bioamp
Alphabet’s X details Project Amber, a quest for a single biomarker for depression that fell short of its goal (TechCrunch):
Alphabet’s X (the Google-owner’s so-called “Moonshot Factory”) published a new blog post today about Project Amber, a project it’s been working on over the past three years — the results of which it’s now making available open source for the rest of the mental health research community to learn from, and hopefully build upon.
The X project sought to identify a specific biomarker for depression — it did not accomplish that (and the researchers now believe that a single biomarker for depression and anxiety likely didn’t exist), but X is still hoping that its work on using electroencephalography (EEG) combined with machine learning to try to find one will be of benefit to others … What is perhaps most notable about this pursuit, and the post today that Alphabet released detailing its efforts, is that it’s essentially a story of a years-long investigation that didn’t work out — not the side of the moonshot story you typically hear from big tech companies.
In fact, this is perhaps one of the best examples yet of what critics of many of the approaches of large tech companies fail to understand — that some problems are not solvable by solutions with analogs in the world of software and engineering.
The announcement:
Sharing Project Amber with the mental health community (X blog post):
Today at the Sapien Labs Symposium, my colleague Vlad Miskovic presented insights from Project Amber, an early stage mental health project at X. Amber’s small team of neuroscientists, hardware and software engineers, machine learning researchers and med-tech product experts have been developing prototype technologies to help tackle the huge and growing problem of mental health. After three years of exploration, we recently wrapped up our work at X. Now we are making our technology and research findings freely available in the hope that the mental health community can build upon our work…
Here are three key insights from our user research:
- Mental health measurement remains an unsolved problem. Despite the availability of many mental health surveys and scales, they are not widely used, especially in primary care and counseling settings. Reasons range from burden (“I don’t have time for this”) to skepticism (“Using a scale is no better than using my clinical judgement”) to lack of trust (“I don’t think my client is filling this in truthfully” and ”I don’t want to reveal this much to my counsellor”). These findings were in line with the literature on measurement-based mental health care. Any new measurement tool would have to overcome these barriers by creating clear value for both the person with lived experience and the clinician.
- There is value in combining subjective and objective data. People with lived experience and clinicians both welcomed the introduction of objective metrics, but not as a replacement for subjective assessment and asking people about their experience and feelings. The combination of subjective and objective metrics was seen as especially powerful. Objective metrics might validate the subjective experience; or if the two diverge, that in itself is an interesting insight which provides the starting point for a conversation.
- There are multiple use cases for new measurement technology. Our initial hypothesis was that clinicians might use a “brainwave test” as a diagnostic aid. However, this concept got a lukewarm reception. Mental health experts such as psychiatrists and clinical psychologists felt confident in their ability to diagnose via clinical interview. Primary care physicians thought an EEG test could be useful, but only if it was conducted by a medical assistant before their consultation with the patient, similar to a blood pressure test. Counsellors and social workers don’t do diagnosis in their practice, so it was irrelevant to them. Some people with lived experience did not like the idea of being labelled as depressed by a machine. By contrast, there was a notably strong interest in using technology as a tool for ongoing monitoring — capturing changes in mental health state over time — to learn what happens between visits. Many clinicians asked if they could send the EEG system home so their patients and clients could repeat the test on their own. They were also very interested in EEG’s potential predictive qualities, e.g. predicting who is likely to get more depressed in future. More research is needed to determine how a tool such as EEG would be best deployed in clinical and counseling settings, including how it could be combined with other measurement technologies such as digital phenotyping.
News in Context:
- Machine-learning study finds EEG brain signatures that predict response to antidepressant treatments
- What’s normal? When it comes to the brain, it’s hard to say, and that’s why we need to study global neurodiversity
- A call to action: We need the right incentives to guide ethical innovation in neurotech and healthcare
- New report: Empowering 8 Billion Minds via Ethical Development and Adoption of Neurotechnologies
- 10 highlights from the 2019 SharpBrains Virtual Summit


